Optical Coherence Tomography in Neurological Disorders (OCT)
As part of the Sastry Foundation Advanced Imaging, the Optical Coherence Tomography (OCT) has been implemented into the Neurology department. We use the Heidelberg Spectralis SD OCT as an up and coming technique in the neurological field used to gain insight into the retinal structure and to assess atrophy of the nerves in relation to many neurological conditions. While the main focus has been on Multiple Sclerosis, the high resolution and high reproducibility of the OCT holds the potential to increase our understanding of Parkinson's disease, Alzheimer's disease and other conditions seen in clinical Neurology.
Optical Coherence Tomography (OCT) is a noninvasive and quick cross-sectional imaging technique that uses low-coherence interferometry, which is similar to ultrasound imaging except that it uses light instead of sound, to obtain images of the retina. The OCT functions as a type of optical biopsy to produce either a single line two dimensional image of the 10 layers of the retina and part of the choroid, or a multiple line three dimensional image of the macula to assess anatomical changes or of the optic nerve head to determine if there is swelling. This high resolution reconstruction of retinal anatomy takes minimal time to acquire and can be reviewed within minutes. The Spectralis OCT contains a TruTrack active eye tracker which reduces noise to improve the image quality and also allows for AutoRescan, which automatically places follow up scans directly in the same location as the original image, improving our ability to track changes within a patient's retina and bypassing operator variability.
Axonal and neuronal degeneration are commonly associated with a variety of disabilities in many neurological disorders. Within the central nervous system, the retina is unique in that it contains axons and glia, but no myelin and therefore holds the potential to give insight into the effects of neurodegeneration, neuroprotection and possibly neurorestoration. Having this quick processing tool holds the potential for increasing our comprehension of neurodegeneration and its association with specific disabilities in neurological diseases.
-
OTC in Multiple Sclerosis
Multiple Sclerosis (MS) is a neurological inflammatory disease that causes many symptoms, including physical and cognitive impairments, by damaging the protective cover of the nerve (myelin). MS often presents with Optic Neuritis, an inflammation of the Optic Nerve, which is the pathway of the nerves between the eye and the brain. While this can be resolved with treatment, and often the patient's vision returns to close to baseline, there may be lasting damage to the nerves that were effected.
The retina holds the potential to be a "window" into the brain, as it contains unmyelinated neurons and axons. For MS, the most important layer is the top layer, or the Retinal Nerve Fiber Layer (RNFL) because it is associated with unmyelinated axons. OCT images have shown correlations between thinning in the RNFL and clinical outcomes in MS, even in patients who have never experienced attacks of Optic Neuritis. Monitoring of retinal fiber thinning is proving useful in tracking the progression of the disease in MS, and OCT is becoming a more widely used clinical tool here in the Neurology Department.
What our lab is investigating
- OCT RNFL thinning, difference among races with MS
- MS and the presence of Microcystic Macular Edema in relation to disease severity
- Correlation of OCT outcomes and MRI outcomes in MS patients
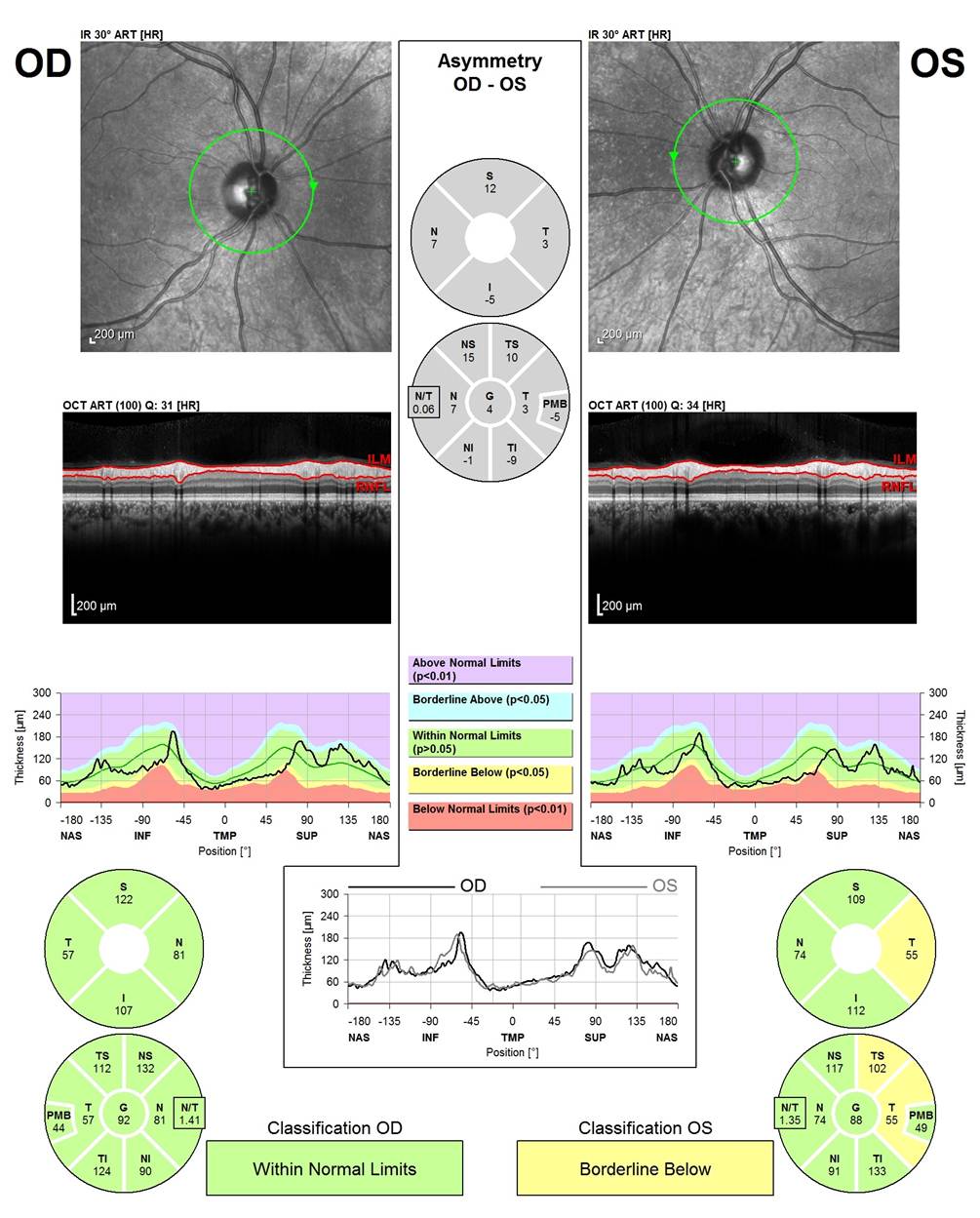
Top image: The green line indicates the location of where the OCT image is taken around the Optic Nerve Head (ONH)
Second Image: The OCT scan is automatically segmented between the two red lines (the internal limiting membrane to the Retinal Nerve Fiber Layer (RNFL))
Third Image: The black line indicates the RNFL thickness for this patient. Color coding is as indicated between the two graphs.
Bottom: Pie charts indicate sector thickness in the nasal, temporal, superior and inferior areas around the ONH, indicating borderline thinning in the temporal segment in the left eye.
-
OCT in Parkinson's Disease
Parkinson's disease (PD) is a degenerative disorder associated with death of dopamine producing cells within the brain which results in motion disorders, like tremors.
PD can also cause visual symptoms associated with spatial contrast sensitivity, motion perception abnormalities, color deficiencies and visual hallucinations. Past studies have found dopaminergic neuronal cells within the third layer of the retina, the inner plexiform layer, drawing a link between PD and the retina. Initial observations of PD and OCT found no significant differences in the Retinal Nerve Fiber Layer thickness as compared to healthy age matched controls, however macular volume was noticed to be thinner than average, indicating loss within another layer.
We are collecting data to evaluate any correlations between macular thinning, specifically in the ganglion cell layer and inner plexiform layer of the retina and progression in Parkinson's Disease. We plan to use the OCT outcomes to increase our knowledge of the disease as it relates to clinical progression and presentation, and to hopefully aid in the diagnosis of this disease.
Currently we have found coronations with thinning of the macular volume, and with segmentation of the layers, we discovered significant loss of volume within three of the layers along with significant thickening in one. This data is in the process of being published.
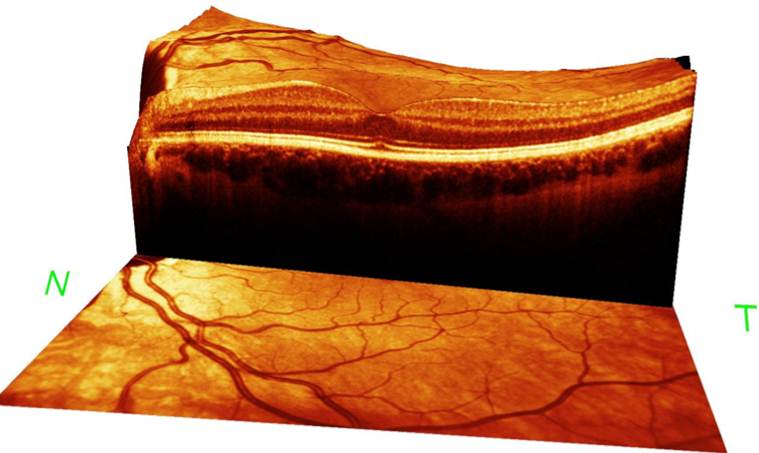
3D reconstruction of the macula, including the 10 layers of the retina and part of the chorioid. Image taken using the 61 line posterior pole scan
OCT in Other Neurological Disorders
- The retina, when viewed for its structure, holds the potential to be a window into the brain on many neurological disorders. While information is abundant for MS and increasing for PD, other neurological-linked disorders can still be investigated to increase our understanding and the OCT presents as a high resolution, highly reproducible tool available to do just that.
Chronic Relapsing Inflammatory Optic Neuritis (CRION)
CRION is a rare disorder which presents as an optic neuritis that relapses (worsening of or reoccurrence of the symptoms after a period of improvement) over a period of time, often with severe and lasting effects of vision loss.
Understanding patterns within the OCT outcomes holds the potential to assist in diagnosis or help track progression of patients with CRION. We are currently continuing to follow patients, both after initial attack of ON to see if they have relapses over time, and on patients that have remitting attacks of ON with negative NMO antibodies to assess patterns within the RNFL outcomes.
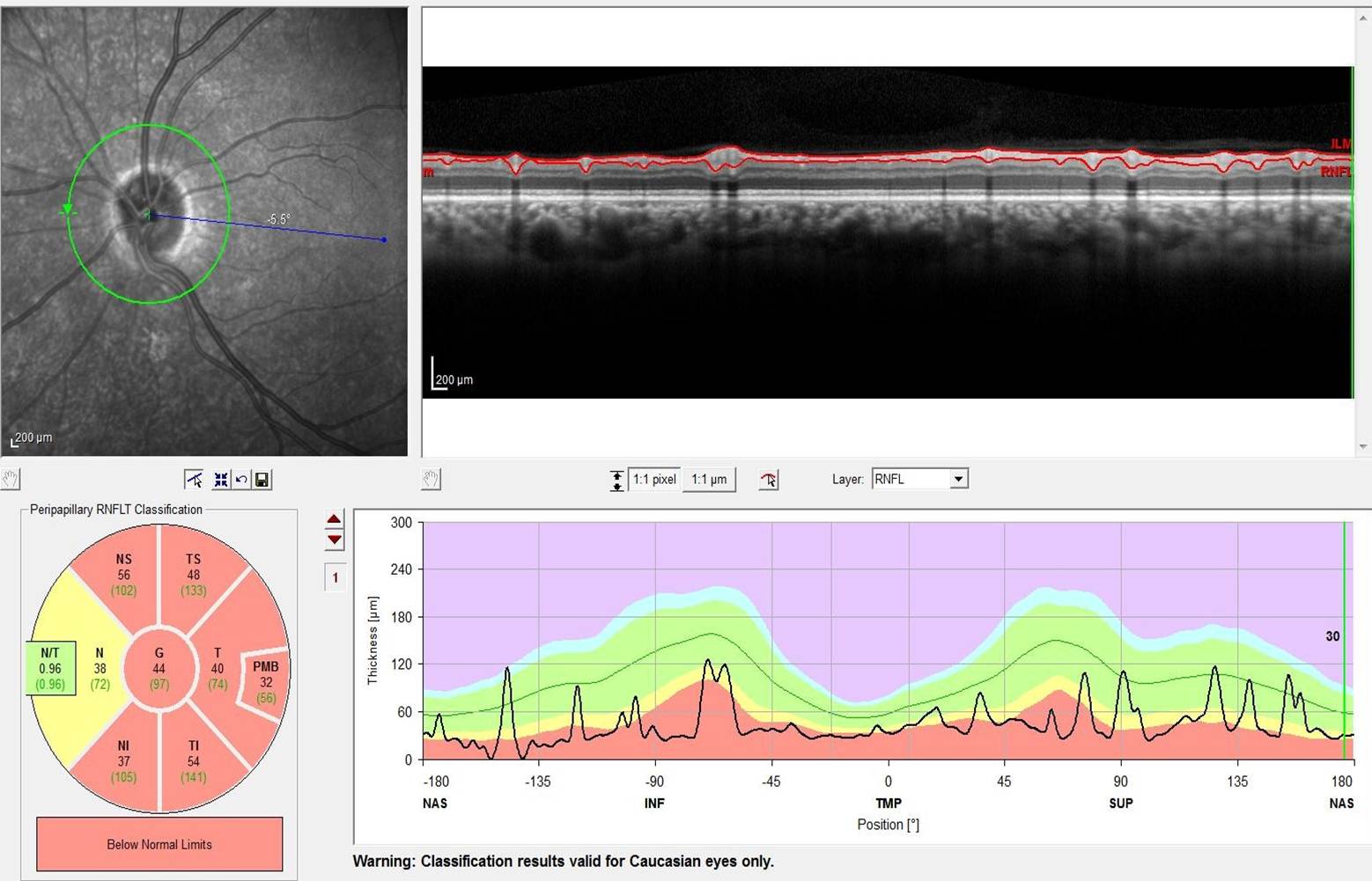
RNFL outcomes for CRION patient.
Top left: Green circle indicates where the image was taken around the optic nerve head.
Top right: the circular image around the ONH is flattened out and flipped 90 degrees so that all layers of the retina can be observed. The RNFL is being measured between the two red lines.
Bottom left: Red coloring within the pie chart is showing significant thinning in all segments, except the nasal, which is borderline below average.
Bottom right: the green section indicates the average thickness of the RNFL associated with this person's age group, the black line indicates the actual thickness of the RNFL for this person.Alzheimer's Disease
In Alzheimer's disease, we are investigating the potential to find biomarkers within the retina that will aid in early diagnosis of the disease. As a disease that requires a diagnosis of exclusion, having a tool which could assist in early diagnosis will be beneficial for treatment and control of the development of the disease. If a trend is found, OCT may also prove useful as a secondary outcome to see the efficacy of medications and treatments over time.
Pediatrics
While OCT has become a useful tool in the MS population in adult patients, this technique has not been used to examine children with acute demyelinating encephalomyelitis (ADEM), isolated optic neuritis or transverse myelitis and thus comparisons based on adult and pediatric onset forms have not been made. Comparisons between age populations have also not been made in individuals with MS or NMO. We plan to collect data on patients over time and correlate with disease severity and progression.
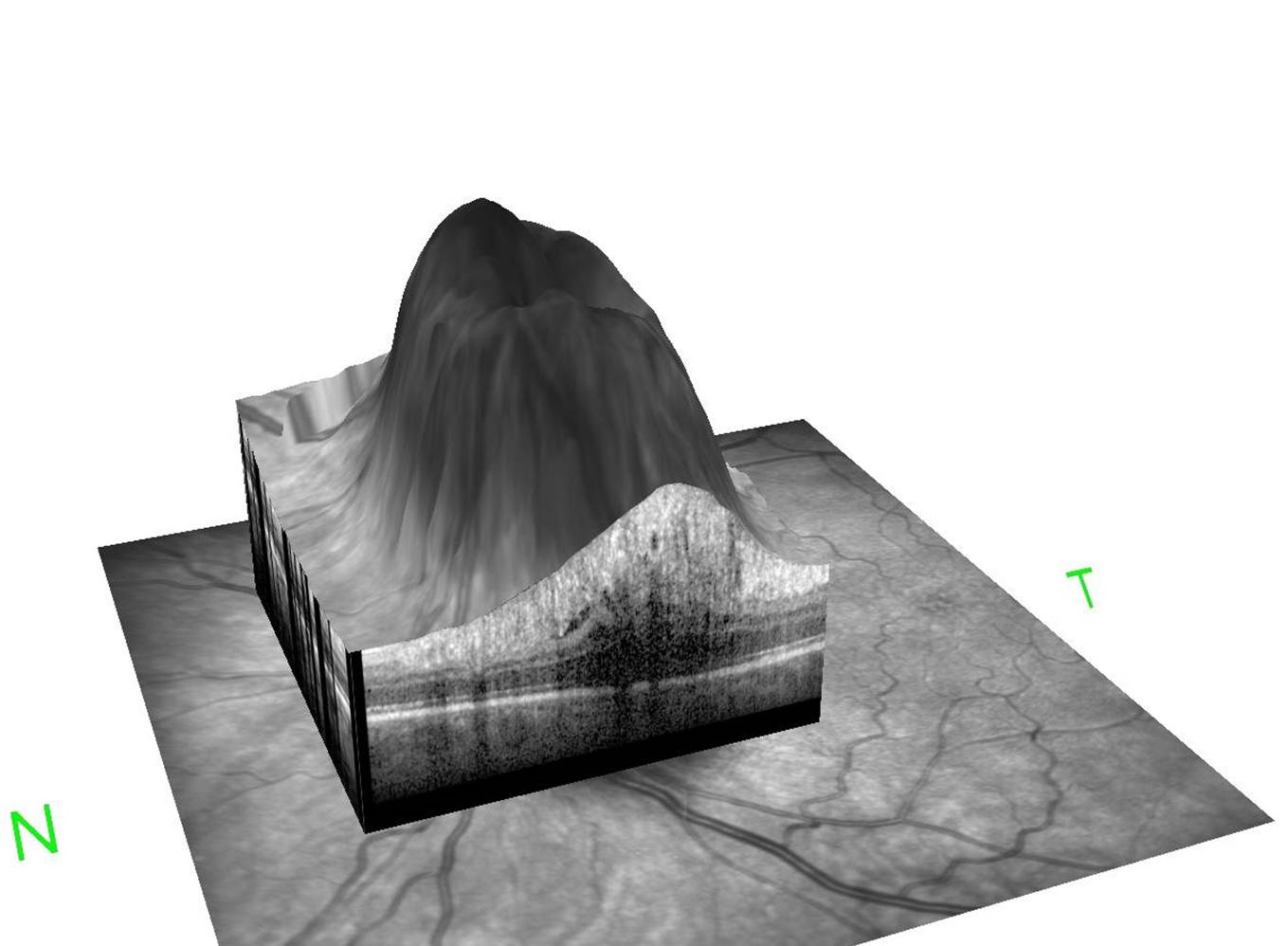
32 line image 3D- reconstruction of swelling of the optic nerve head - The retina, when viewed for its structure, holds the potential to be a window into the brain on many neurological disorders. While information is abundant for MS and increasing for PD, other neurological-linked disorders can still be investigated to increase our understanding and the OCT presents as a high resolution, highly reproducible tool available to do just that.
